By Carolyn Bick
NORTHWEST ASIAN WEEKLY
As measles cases surge across the country, topping more than 1,300 cases as of March 11, the United States is poised to lose its status in the world as having eradicated the disease in-country. The U.S. has held that status since 2000.

Dr. Tao Kwan-Gett
Washington hasn’t been spared—in fact, cases here continue to climb and already sit at more than twice the level they were last year at this time, State Health Officer Tao Sheng Kwan-Gett with the Department of Health (DOH) noted in an interview with the Northwest Asian Weekly. This is primarily because of misinformation and disinformation spreading about the measles vaccine (the MMR vaccine), which means that people don’t get themselves or their children vaccinated and therefore spread the disease. The state has already reported 26 official measles cases, and Kwan-Gett said Washington can expect cases to climb, as people visit Washington from other states.
“It used to be that our main concern was people traveling internationally or visitors from other countries where there’s measles,” Kwan-Gett said. “People need accurate information on vaccines to make good health decisions for them and their families. When there’s misinformation and disinformation, that makes it hard for people to trust the information that they’re getting when they are hearing conflicting messages.”
Possible loss of eradication status
In addition to other variables, a country can lose its status as having eradicated measles if an outbreak lasts for 12 months and an outbreak can be linked to the same strain of the virus. This suggests that the outbreak source is domestic, and therefore circulating amongst the population, rather than documented cases imported from outside the country.
Earlier this year, for instance, the United Kingdom lost its status as having eradicated measles, after it was determined that less than 95% of the population was vaccinated against the disease and there were more than 1,000 confirmed measles cases in 2025 and 3,600 suspected cases in 2024.
The World Health Organization (WHO)’s Americas arm, the Pan-American Health Organization (PAHO), administers and revokes eradication designations, and was set to meet in April to determine whether the U.S. should lose that designation. However, that meeting has been delayed until November, after the midterm elections.
The WHO has pushed back against speculations that the decision to delay the meeting was politically motivated, even though the PAHO wants to retain the U.S. as a partner, despite President Donald Trump pulling the U.S. out of the WHO in 2025. The U.S. officially exited the WHO on Jan. 22 of this year.
So, who’s at highest risk?
While anyone who is not vaccinated can catch the disease, socioeconomic and demographic factors can make people more susceptible to contracting measles, Kwan-Gett said. Immigrants are particularly at risk, because many come from countries where measles is endemic, which means that the disease is constantly circulating.
“They’re more likely to have family or friends visiting from those countries, and they might be infected with measles, or they might be more likely to travel back to their home country and become infected with measles,” Kwan-Gett explained. “Or they might get immunized if they knew about the dangers of measles and knew about [MMR] vaccine, but if they don’t have health education materials in their language, they don’t speak English, or if they don’t have access to a healthcare provider who can communicate with them in their language.”
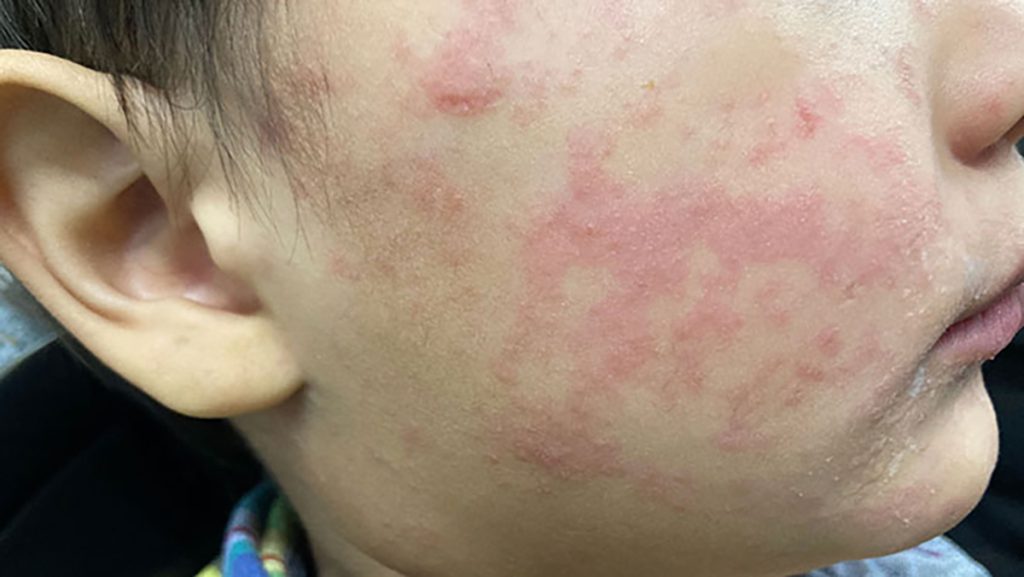
The child’s cheek shows the characteristic rash associated with measles. (Photo from CDC.gov)
Another socioeconomic factor, he said, is that people may not have ready access to healthcare or a primary care provider, or may not have a job that allows them to easily take time off work to get themselves or their children vaccinated.
“Access to care can also increase your risk to measles by impacting whether you’re vaccinated or not. It’s more of an issue worldwide,” Kwan-Gett said. “Poverty and malnutrition can increase a child’s risk of dying from measles. So many people don’t know that in 2024, there were 95,000 deaths due to measles worldwide. Most of these occurred in children, and many of these children had poor nutrition that made them more vulnerable to measles and also maybe did not have access to measles vaccine.”
Living in a crowded or multigenerational household can also increase risk, because the disease can spread more easily in close living quarters.
Community vaccination statistics
DOH spokesperson Trevor Christensen later sent the Northwest Asian Weekly statistics on vaccination rates amongst Asian Americans, Native Hawai’ians, and Pacific Islanders. The data indicates that “children identified as non-Hispanic Asian may have slightly higher rate of MMR coverage while non-Hispanic Native Hawaiian or Other Pacific Islanders tend to have lower or middling coverage.”
However, Christensen noted, the disparities in vaccination rates may be due to one-time vaccinations, which disappear as children age.
“So, perhaps Asian children are more likely to be vaccinated on-time or even early,” he explained. “MMR vaccination (or documented exemptions) are required to attend school in Washington, so, as kids get older, they experience this uniform policy pressure to comply with state law, get catch-up vaccinations, and many of these disparities may disappear in older age cohorts. … If kids who tend to get vaccinated also have a higher rate of being reported as Asian, this could also drive apparent disparities.”
He also stressed that the registry only records those who have been vaccinated, “making it a poor data source for making inferences about who has not been vaccinated. We don’t have demographic information that lets us identify specific ethnic communities with low coverage rates which may exist within the monolithic “Asian” or other race categories and, even if we did, if they are not getting vaccinated, these communities may not be well represented in the registry if at all.”
A possible influx
One of the major events coming down the pipeline that University of Washington Medicine Drs. Shireesha Dhanireddy and Alex Greninger said during a media briefing may bring an influx of measles to the state is the World Cup games, in addition to cruises and air traffic already coming into the U.S.

Dr. Shireesha Dhanireddy, UW Medicine’s Associate Chief Medical Officer, during a media briefing about measles on March 11, 2026
“Those are all signs of potentially more cases to come,” Greninger said. “We also know that our vaccination coverage is still too low. We’re below the median level in the United States. We’re below the level that creates herd immunity.”
Dhanireddy emphasized that the World Cup games will make contact tracing—tracing the path of a disease to better alert people who may have been exposed—extremely difficult. Often, tracing even just one person is difficult, she said, because they usually initially think their symptoms are that of a different viral illness.
“In that time, they’ve been to many, many places … where there may be a high populations of people, and then our public health has to go and find out where exactly this person has been, who they’ve been in contact with. Once they’ve identified those potential contacts, they have to determine immunization status to see are they really at risk for getting sick from measles and then going on to spread it themselves,” Dhanireddy explained. “I’s a huge amount of work that has to happen. And the more cases we have, the more work that’s got to be done. And that’s when we think about the World Cup coming here. That’s a huge stadium full of people. That’s really not possible to do targeted contact tracing when it’s just essentially the entire population that we’re talking about.”
Symptoms and long-term consequences of infection
Measles is a particularly destructive disease. Once a person catches it, their immune system can “forget” its defenses, making a person more vulnerable to infection from those diseases they have already been vaccinated against, Greninger explained. These can be deadly or have lasting, long-term consequences that vaccines—inert versions of a disease to “teach” the immune system—don’t carry.
“You basically have to get revaccinated … because it just knocked out all of your memory immune cells, because that’s the cell that it amplifies in,” Greninger said. “That’s a very unique feature to measles that really no other virus replicates.”
Fortunately, unlike other viral illnesses that require yearly vaccination, like COVID, Greninger said, measles doesn’t really change. This makes it entirely possible to wipe out the disease through vaccination.
Common symptoms of measles include a rash, runny nose, and fever, all of which can show up after a person is contagious.
Measles also carries with it the possibility of developing subacute sclerosing panencephalitis (SSPE) up to 15 years after infection. There is no cure for SSPE, and it is almost always fatal. About 10 years ago, researchers found SSPE was more common than initially thought, with about 1 in 609 unvaccinated children under 12 months old and 1 in 1,367 unvaccinated children under 5 developing it, years after infection.
Measles can also be contagious up to four days before a person starts to show symptoms, and the virus—which is primarily airborne, though can also show up in a person’s urine—can linger in the air for about two hours after a person has left the room. This makes the disease very hard to control, Kwan-Gett said.
Getting accurate information
Public health officials say misinformation about vaccines can contribute to lower vaccination rates.
U.S. Health and Human Services Secretary Robert F. Kennedy Jr. has long questioned vaccine safety and promoted claims rejected by public health experts. His past involvement in Samoa has also drawn scrutiny following a 2019 measles outbreak that sickened thousands and killed 83 children, many under age 5.
Kwan-Gett said to get accurate information from a trusted healthcare provider. He also said that pharmacists can provide guidance, and that vaccinations are available at pharmacies or health care clinics.
“The most important thing to know is that the [MMR] vaccine is our best protection against measles infection,” Kwan-Gett said. “It’s one of the most well-tested and most effective vaccines around. And the more that we can get people vaccinated against measles and the higher proportion of people within our community and our state that get vaccinated, then the lower the likelihood that we’ll have cases of measles or outbreaks of measles in our communities here in Washington.”
For more information, visit the DOH’s website. The department offers basic measles information in 18 different languages, and offers MMR vaccines for children under 18 years old at no cost. The MMR vaccine protects against measles, mumps, and rubella. You can get the MMR vaccine at most Washington pharmacies or clinics.

